Created a pan-Canadian Network of leading cancer centres

In 2019, the Government of Canada announced a landmark investment to accelerate precision oncology and transform how cancer is studied and treated across the country. This investment helped us launch Phase 1 of the Marathon of Hope Cancer Centres Network, a bold, pan-Canadian initiative led by the Terry Fox Research Institute and the Terry Fox Foundation.
From the beginning, our mission was clear: to unite Canada’s cancer research and care communities under a single, powerful vision—one that helps improve outcomes and quality of life for cancer patients across Canada and get us closer to finishing the marathon against cancer that Terry Fox began in 1980.
The results have been astonishing. Over the last five years, more than 1,300 collaborators from across the country have come together to create and deploy a national strategy to accelerate precision oncology research in Canada. Together, we are expanding access to state-of-the-art cancer care while building a shared framework for data-driven discovery that will reshape cancer research and care for generations to come.
As Phase 1 of this initiative comes to an end, it’s time to share what we’ve collectively accomplished. This Innovation Report captures the Network’s growing impact—highlighting the milestones achieved, the lessons learned and the foundation we’ve built for the next phase of the Network’s journey.
Cancer is the leading cause of death in Canada. Despite major advances over the last few decades, two in five Canadians will be diagnosed with cancer in their lifetime, and one in four will die from the disease.
In recent years, a new framework for cancer care known as precision oncology has emerged as a promising way to improve outcomes and quality of life for cancer patients. This new paradigm moves away from one-size-fits-all treatments based on a cancer’s anatomic site of origin and focuses instead on tailoring treatments to the unique biology of each patient and of their cancer. But while precision medicine is already improving outcomes for some patients, a lot of research still needs to be done to bring it to more patients across the country.
On its own, no single cancer centre has the data or resources to accelerate precision oncology research and care in ways that will benefit all Canadians. That is why the Marathon of Hope Cancer Centres Network is uniting cancer research and care institutions across the country in an unprecedented collaboration for the benefit of cancer patients everywhere.
The Network has created a unified national strategy to accelerate research, share data and translate discoveries into clinical care more quickly. Inspired by Terry Fox’s vision, the Network is building a national, patient-centred approach to precision oncology—so the breakthroughs of today can become the standard of care tomorrow for more Canadians, no matter who they are or where they live.
Just as everyone’s DNA is unique, each person’s cancer also has a distinct molecular profile. For example, two breast cancers that look similar under a microscope can be driven by different genetic mutations, making them respond differently to treatment.
Today, cancers are most often treated according to their location in the body. Precision oncology, on the other hand, is based on the idea that an individual patient’s treatment can be guided by their unique characteristics, including their tumour’s individual molecular signature. For example, patients whose tumour cells carry a mutation in a specific gene may receive a drug that acts against that mutation, instead of a “one-size-fits-all" chemotherapy. This helps personalize treatments, so that each patient receives the right drug at the right dose at the right time.
Learn more about precision medicine for cancer by clicking here.
Since its inception in 2007, the Terry Fox Research Institute has invested in highly collaborative scientific teams doing groundbreaking research for the benefit of cancer patients. This unique investment strategy has allowed us to unite leading cancer researchers across Canada, allowing them to work together like never before to tackle some of cancer’s biggest challenges. The Marathon of Hope Cancer Centres Network is a built on these collaborations.
Below is a timeline of activities for the Marathon of Hope Cancer Centres Network:
April: After years of consultation with the Canadian research community, TFRI begins brand and marketing groundwork to support a future pan-Canadian cancer research network inspired by Terry Fox’s Marathon of Hope.
February: Network Pilot projects begin, testing early models for multi-centre collaborations and data-driven cancer research.
April: Terry Foxer campaign engages supporters and reinforces the connection between Terry Fox’s legacy and a new vision for cancer research.
February: MOHCCN is funded in the federal budget, marking a critical milestone in establishing the Network.
April: Public launch of the Network’s vision in Newfoundland and Labrador, underscoring the Network’s pan-Canadian scope.
April to December: National workshops bring researchers, clinicians and partners together to shape priorities and create a unified governance structure.
June: TFRI and partners submit official proposal to Health Canada, solidifying deliverables for Phase 1 of the Network.
June: Invitations go out to founding members in Ontario, Quebec and British Columbia to submit designation applications, initiating the process to officially form the Network.
June: Network operations officially begin as TFRI and Health Canada sign a contribution agreement.
June-December: Centres ramp up participation and operational capacity.
December: Prairie Cancer Consortium receives designation.
January: Fully operational management infrastructure established to support national coordination through TFRI.
January: Atlantic Cancer Consortium receives designation, meaning that the Network now connects centres from coast to coast.
April: Year of Data Acceleration is launched, focused on advancing data generation.
May: Patient Working Group (PWG) is launched to incorporate patient voices at all levels of the Network.
February: Phase 2 campaign begins, with an aim to sustain and expand the Network’s impact.
April: Year of Capacity Building is launched to strengthen research and data capabilities at participating centres, particularly smaller centres.
September: Patient Voices in Research launched, firmly embedding patient perspectives into Network activities and decision-making.
February: FINISH IT campaign launched, reaffirming Terry Fox’s vision and rallying national momentum. The Network adopts this vision as a rallying call to achieve the ambitious goals it set out for itself in Phase 1.
July: Final Phase 2 proposal submitted to Government of Canada to support expansion and long-term sustainability.
August: 10,000 cases reached, reflecting the scale of data generation across Canada.
August: Network grows to more than 50 member institutions.
September: Network data sharing begins, enabling pan-Canadian research and discovery.
November: Government of Canada includes funding for Phase 2 in the 2025 Federal Budget approved on Nov. 17.
March: 15,000-case Gold Cohort completed
TBD: Phase 2 launch, advancing the Network’s mission to accelerate precision oncology and improve outcomes for patients across Canada.
We’ve categorized the impact of Phase 1 into five major achievements. Click on any title to navigate to each section:

Photo of Terry Fox by Gail Harvey
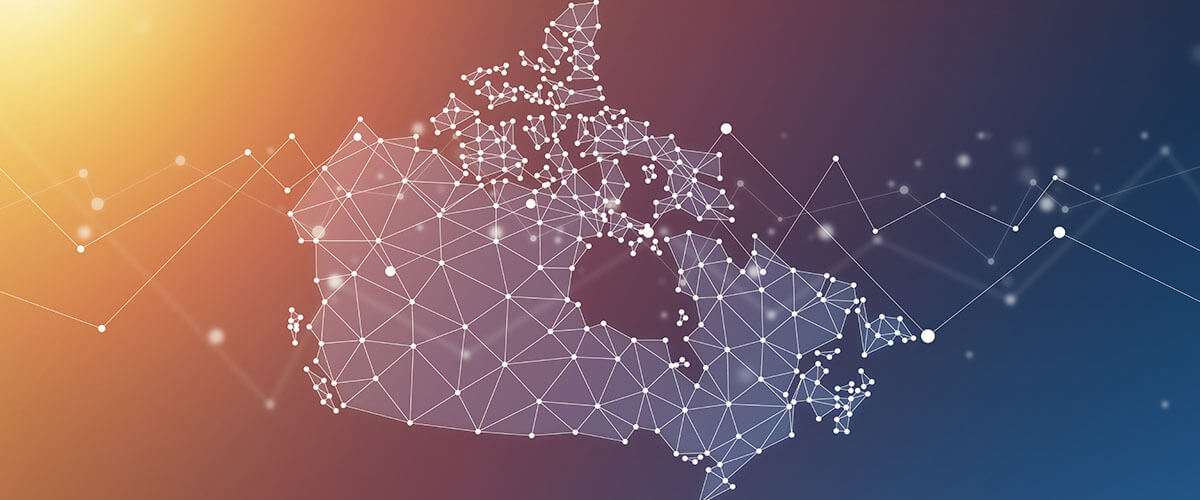
Inspired by Terry Fox, over the last five years the Marathon of Hope Cancer Centres Network has united patients, researchers, clinicians, administrators and donors from institutions across the country in an unprecedented collaboration for the benefit of all cancer patients in Canada. This Team Canada of Cancer Research has created and deployed a national strategy to accelerate precision oncology research and care, getting us closer to the day when all cancer patients in Canada have access to personalized treatments, no matter who they are or where they live.
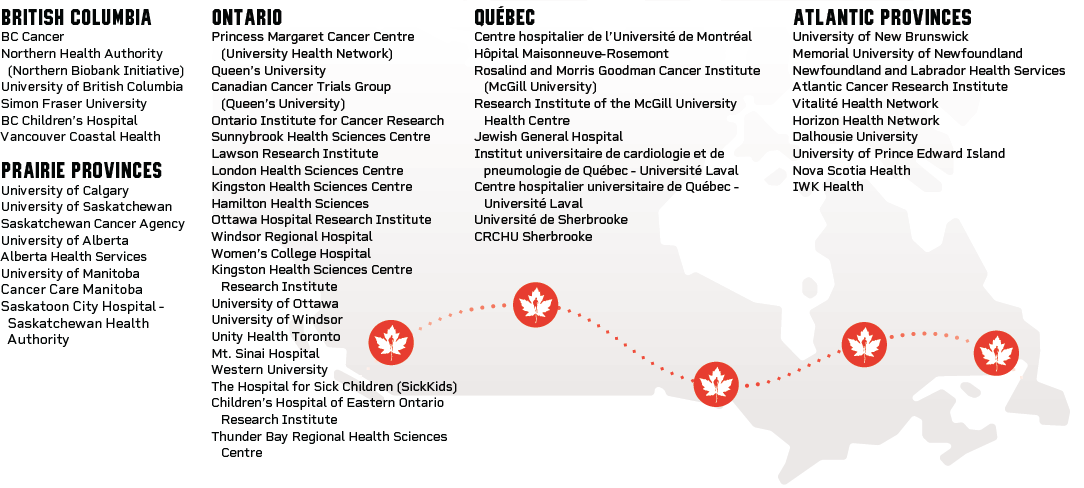



The Network currently includes more than 50 member institutions, over 1,300 individuals and greater than 100 research and funding partners from across Canada. It is anchored by five regional consortia representing all ten provinces. From west to east, these are: the BC Cancer Consortium (BC2C), the Prairies Cancer Consortium (PR2C), the Ontario Cancer Consortium (OCC), the Marathon of Hope - Québec (MOH-Q) consortium, and the Atlantic Cancer Consortium (ACC).
Member institutions
Over 50 universities, hospitals, research institutes, healthcare authorities and cancer centres have joined the Network as official members. These members sign agreements called Joinders, which allow funds to flow from the Network to these institutions. By signing on, institutions also agree to make Network data available to researchers across the Network for academic, non-commercial studies
MOHCCN Partners
The Network currently has over 100 funding and research partners. These institutions participate in, collaborate on and/or co-fund certain Network activities and may have researchers associated with the Network, but are not full Network members. Partners may have an official agreement with a Network Member Institution, but no official agreement with the Network itself. In many cases, these institutions provide matching funds for Network projects.
MOHCCN Individual Members
Patients, researchers, oncologists, bioinformaticians and administrators can also join the Network as members by contributing to Network activities and/or receiving Network funds, as outlined in the MOHCCN Individual Membership Policy. Individual members may be affiliated with a MOHCCN Member Institutions and/or Partner.
An up-to-date list of member and partner institutions can be found here
The Network continues to grow, and new members and partners are encouraged to join the Team Canada of Cancer Research.
Network members, affiliates and partners join the 'Team Canada of Cancer Research’, working together to accelerate precision oncology across Canada to improve outcomes and quality of life for all cancer patients. Benefits of being a Network member include:
Novel opportunities for local and cross-country interdisciplinary collaborations
Opportunities to shape Canadian cancer research as well as the delivery of personalized, precision cancer care across the country
New sources of funding for precision oncology research, supporting a wide range of projects from genomic profiling and data studies to health technology assessments, patient-reported outcomes studies and social science investigations
Priority access to Gold Cohort data





“The working relationships that are formed through the Marathon of Hope Cancer Centers Network are how we are going to cure cancer. We are leveraging the skills, knowledge and energy of the entire country right now, and I believe this is the way to make Terry’s dream a reality.”
- Dr. Laura Hopkins, oncologist at the Saskatchewan Cancer Agency and professor at the University of Saskatchewan’s College of Medicine
Over the last five years, the Network has united Canada's leading researchers and oncologists in precision oncology to create the Team Canada of Cancer Research. Read the stories below to learn more about what some of these incredible individuals have to say about the groundbreaking work they're doing thanks to Network funding.

Precision oncology has the potential to transform cancer care, allowing patients to receive specific therapies targeted to the exact mutations that cause their cancer, thus improving their outcomes and quality of life. But today, only a small subset of patients benefits from this new approach to cancer care.
To make precision medicine a reality for more cancer patients, clinicians and researchers need to better understand how cancer is formed in each person, why certain patients respond differently to similar treatments and how to best target the unique vulnerabilities in each patient’s cancer. And for that they need access to data—more than any single cancer centre in Canada can generate on its own.
That’s why the Marathon of Hope Cancer Centres Network set out to create the MOHCCN Gold Cohort, Canada’s largest and most complete cancer case resource. This game-changing national resource has the potential to transform how cancer is studied and treated here and around the world, now and into the future.


One of the main deliverables of the first phase of the Network was the creation of a national data resource that included high-quality genomic and clinical data from 15,000 diverse cancer patients treated across the country: the MOHCCN Gold Cohort.
This comprehensive, consistent and high-quality data resource is meant to bolster innovation and precision oncology research across Canada and beyond. Data from the Gold Cohort are available to Network researchers, and the development of the dataset has helped the Network establish accessible and secure data sharing methods, procedures and infrastructure.
To enable cancer research and care innovations that benefit all cancer patients across Canada, the Gold Cohort dataset must reflect the full spectrum of this country’s diverse populations. Over the course of Phase 1, the Canadian Spectrum Working Group has developed and promoted strategies to include equity-deserving communities and populations within Network activities, including the Gold Cohort dataset.
The MOHCCN Gold Cohort brings together comprehensive genomic and clinical data from 15,000 cancer patients across Canada. For each patient (or ‘case’), it includes:
Together, these data allow for researchers to get the most complete view of a cancer’s DNA and RNA possible with technologies available today, capturing both known and yet-to-be-discovered features of tumour biology; better understand what genetic alterations are present in a patient’s cancer cells and which may have been inherited; and explore how molecular characteristics influence disease progression and treatment response in people with cancer.
The result is a unique resource that makes possible investigations into how cancers arise, progress and respond to treatments—and how this information can be leveraged to provide personalized cancer care to patients across Canada.
To populate the Gold Cohort, the Marathon of Hope Cancer Centres Network is funding more than 140 projects focused on data generation in over 50 partner institutions across Canada.
These projects have been selected due to their ability to generate data according to the stringent technical and legal guidelines established by the Network and add both prospective (newly diagnosed) and retrospective (already diagnosed with samples available through a biobank) cases to the Gold Cohort. Informed patient consent to their samples and data being used in a research setting is required for all cases.
In practice, there are two main types of projects currently adding cases to the Gold Cohort: regional consortia projects and pan-Canadian projects. Regional consortia projects are approved at the consortium level, while Pan-Canadian projects – which bring together researchers from across the country – were awarded after an expert review panel assessed applications submitted through a call for proposals.
As we continue to implement our standards and build the infrastructure needed to collect, curate and share data across the country, it is the Network’s vision to expand beyond this current model, so that any patient across the country wanting to donate their data to the Network will be able to easily enroll in an MOHCCN-supported study to do so.
Learn more about Network-funded projects by clicking here.
The MOHCCN Gold Cohort was conceived within a rapidly evolving global cancer genomics landscape shaped by nearly two decades of large-scale international collaboration. Early landmark initiatives such as The Cancer Genome Atlas and the International Cancer Genome Consortium (ICGC) established the molecular foundations of cancer research, while later efforts—including the ICGC’s Pan-Cancer Analysis of Whole Genomes (PCAWG) project, the Cancer Programme of the UK’s 100,000 Genomes Project, and the Netherlands’ Hartwig Medical Foundation—expanded the use of cancer whole-genome sequencing at scale. Complementary programs such as Project GENIE and ICGC’s Accelerating Research in Genomic Oncology (ARGO) have further accelerated the sharing of cancer genomic data worldwide.
Against this backdrop, the Gold Cohort stands out for its distinctive combination of scale, depth and diversity. Bringing together comprehensive whole-genome and transcriptome sequencing from more than 15,000 patients—linked to detailed, standardized, longitudinal clinical data—the Cohort enables analyses that are not possible in smaller or less integrated datasets.
Its alignment with international standards ensures interoperability, while its representation of more than 40 cancer types, diverse populations, rare cancers and advanced, treatment-resistant disease positions it to address some of the most urgent challenges in oncology. Together, these features make the Gold Cohort a uniquely powerful resource designed to accelerate discovery and help bring precision oncology to all cancer patients in Canada.





“As a genomics scientist, I am inspired by the scale and ambition of this initiative. A truly pan-Canadian effort — integrating data from across provinces through a federated model — is no small task. But it positions MOHCCN and Canada as a global leader in data coordination, the responsible use of AI, and collaborative science.”
-Dr. Catalina Lopez-Correa, Physician, cancer patient and leader in genomics; co-chair of the MOHCCN Patient Working Group.
The MOHCCN Gold Cohort aims to be Canada's largest and most complete cancer case resource. The stories below will help you better understand what the Gold Cohort is, how we built it, and how it compares to other large-scale global genomic initiatives.

Precision oncology cannot advance without bold, strategic investment in research that spans the entire spectrum of cancer: from basic discovery to clinical trials and from capacity building to health system assessment.
Over the last five years, the Marathon of Hope Cancer Centres Network has invested in projects that span this wide range of topics. By funding high-impact projects that align with our shared national strategy, the Network is accelerating the deployment of precision oncology, ensuring that discoveries made in the lab can more rapidly improve outcomes and quality of life for patients across Canada and beyond.

.png?sfvrsn=81ef2106_0)

In Phase 1, the Marathon of Hope Cancer Centres Network (MOHCCN) funded more than 200 projects designed to accelerate the deployment of precision oncology across Canada. These projects fall into one of four major funding buckets:
Creating the MOHCCN Gold Cohort. In Phase 1, the Network created Canada’s largest and most comprehensive cancer case resource. Through joint investments with partners, each case underwent whole-genome and transcriptome sequencing, and matched clinical data was carefully curated. This pan-Canadian effort is generating large-scale genomic and clinical datasets that allow researchers to better understand why patients respond differently to treatments and to identify new, more precise therapeutic targets.
Supporting the next generation of experts in precision oncology. Recognizing that people power progress, Phase 1 funding also supported early-career researchers through the Clinician-Scientist and Health Informatics & Data Science Awards, helping train the next generation of leaders in precision oncology.
Patient Voices in Research Initiative. This first-of-its-kind program created by cancer patients, for cancer patients supports 10 research teams addressing critical gaps in precision oncology identified by cancer patients and survivors.
Special Initiatives. The Network also invested in a number of other projects designed to build capacity for data generation and sharing across the country, develop and test new technologies and investigate how best to deploy patient-centric precision oncology at scale within public healthcare systems with limited resources.
Network investments have bolstered research capacity across Canada in multiple ways.
For one, generating data for the Gold Cohort required significant investment to strengthen local expertise in genomics, data science and research across the country. This was coupled with investments in sequencing, biobanking and data sharing infrastructure. This expanded infrastructure and skilled workforce will serve as a lasting foundation, enabling centres nationwide to deliver precision oncology and support high-quality research more consistently and at scale in the years ahead.
These investments were not limited to centres with existing large-scale research programs and advanced care capabilities; the Network also made strategic investments in capacity at smaller centres across the country serving diverse populations, including rural and remote communities, providing important new opportunities for cancer patients across Canada to participate in research and receive state-of-the-art care. These include, but are not limited to, direct investments in:
Prince George, BC
Kingston, ON
Windsor, ON
Moncton, NB
St. John’s, NL
Beyond direct investments, the Network’s cooperative approach has also led to significant new collaborations both within centres and across centres and provinces. These new partnerships have strengthened relationships between research and clinical teams, helping to bring research into the clinic; enabled an unprecedented level of knowledge sharing, positioning especially smaller centres to advance their capabilities quickly and efficiently by following already-successful models; brought together experts and thought leaders like never before to create national standards and guidelines; and made possible pioneering studies into rare and understudied cancers by enabling pooling of samples and resources.
Learn more about the Network’s impact on small centres like Kingston, ON.
Learn more about how the Network is bringing new hope to patients with rare cancer.
Network-generated data are already advancing research across Canada in two important ways.
First, each of the 144 cohorts generating data for the Gold Cohort can use the genomic and clinical data they generate through Network funding to drive their own research. These investigator-led studies span cancer types, disease stages and scientific questions—leveraging whole-genome and transcriptome sequencing, alongside standardized clinical data, to uncover new biological insights, identify biomarkers and explore mechanisms of treatment response and resistance.
Second, the Network is enabling access to combined Gold Cohort data for research purposes. Through the MOHCCN Data Sharing and Use Pilots, five projects are now accessing cross-cohort Network data, opening the door for Network scientists to leverage the richness and scale of the aggregated dataset to advance research, while testing and providing feedback on the processes and procedures for Network data sharing. This will set the foundation for enhanced access to combined Gold Cohort data in Phase 2 of the Marathon of Hope Cancer Centres Network.






“Programs like the Marathon of Hope Cancer Centres Network’s Clinician-Scientist awards not only help early-career clinician-scientists like me establish our labs and launch our careers—they are pivotal investments in the future of healthcare in Canada.”
- Dr. Ana Nikolic, Clinician-Scientist award recipient (University of Calgary)
Network-funded cohorts and projects are already advancing our understanding of cancer, taking important steps towards improving how we detect, diagnose and treat the hundreds of diseases we call cancer. As projects progress and Network data becomes available, we will see even more findings enabled by the Network.

From its inception, the Marathon of Hope Cancer Centres Network has sought to embed the voices of patients, survivors and caregivers at all levels of its operations. This vision was formalized with the launch of the Patient Working Group (PWG) in 2023. Since then, PWG members have participated in the Network’s governance, its research initiatives and national and regional scientific forums, meaning that individuals with lived experience contribute to Network funding decisions, working groups, conferences and outreach activities across the country. This deep and sustained engagement strengthens the relevance, accessibility and impact of the Network’s work, ensuring that precision oncology in Canada is shaped not only for patients, but with them.

Members of the Patient Working Group during an in-person meeting in Winnipeg (Sept. 2024)

.png?sfvrsn=39dc98ec_0)
The Patient Working Group (PWG) is composed of more than 30 individuals with lived/living experience as cancer patients, survivors and caregivers, hailing from nine provinces.
The group is led by co-chairs who also have lived experience as cancer patients and are involved in cancer research and clinical care: Dr. Catalina Lopez-Correa, founder of The Global Gene, and Dr. Dora Cavallo-Medved, director of the WE-SPARK Health Institute and Associate Dean of the Faculty of Science at the University of Windsor.
Learn more about the Patient Working Group
Patient Working Group members take part in and contribute to various Network activities, including:
Participating in other Network working groups, where they provide unique perspectives and expertise
Developing educational materials related to precision oncology, including for the Network’s Patient Hub
Being active in Network leadership and governance, including contributing to strategic discussions about the Network’s future
Driving the Network’s Patient Voices in Research initiative, a first-of-its-kind funding competition entirely designed and evaluated by the Patient Working Group
Participating in Network conferences and events — for example, PWG members co-chair the Network’s virtual seminar series and co-chair sessions and give presentations at in-person scientific conferences and operational meetings
Acting as ambassadors of the Network in meetings and events with government representatives, donors, media and other stakeholders
Sitting on review panels for other funding programs, such as the Health Informatics & Data Science Awards
The Patient Voices in Research Initiative is believed to be the first of its kind in Canada to be fully designed and adjudicated by cancer patients for cancer patients. It was conceived by the Network’s Patient Working Group, who identified six themes where they deemed gaps exist in precision oncology research:
Equity, access, and disparities related to the continuum of precision medicine care
Clinical trials access
Patient involvement and engagement in precision oncology research
Survivorship care plans and post-treatment resources
Lifestyle interventions in precision oncology
Rare cancers across the age spectrum
After designing, launching and reviewing the awards, the PWG selected 10 outstanding Canadian research teams as recipients of the award. While the original funding envelope was $1M, the quality of the research being proposed was so strong that Network leadership nearly doubled it, and the teams received a total of $1.8M over one year to conduct their research.
As the projects funded through the first round of this innovative funding program come to an end, research teams are preparing to report their findings back to the PWG as well as to the wider Network. Their results will help shape future Network research, and will inform subsequent iterations of the funding initiative.





“We have never come across an initiative that highlights patients, caregivers, and family members as the heartbeat of scientific research to this extent. The Network is a trailblazer in this regard, and we are honoured to be among those funded through this innovative program.”
- Dr. Natasha Szuber, hematologist and project lead at the Hôpital Maisonneuve-Rosemont in Montreal, Quebec
The Network is committed to ensuring that patients, survivors and caregivers help shape cancer research at every level. Read the stories below to meet our Patient Working Group members and learn more about the role they play in bringing precision oncology to more Canadians.
Precision medicine is already impacting the lives of many cancer patients across the country, but we need a national strategy to address the gaps in access and knowledge that prevent more Canadians from benefitting from this potentially life-saving personalized approach.
By establishing a truly national infrastructure that connects cancer centres, harmonizes data collection and fosters collaboration across provinces, the Marathon of Hope Cancer Centres Network is working to close these gaps. Through shared resources, coordinated strategies and a united Team Canada approach, the Network is increasing access to precision oncology across the country — helping ensure that more patients, regardless of who they are or where they live, can benefit from personalized cancer care.


The Gold Cohort dataset is a globally unique resource designed to accelerate discovery, support innovation and ultimately help bring precision oncology to all cancer patients in Canada, improving outcomes and quality of life. It will make possible powerful new studies exploring how cancer is formed in each individual, why certain patients respond differently to similar treatments and how to best target the unique vulnerabilities in each patient’s cancer.
While the full potential of the Gold Cohort dataset will only be realized with time, the research projects fuelling this resource are also bringing benefits to patients now. In fact, more than 140 projects are contributing or have contributed cases to the Gold Cohort — each of these projects is also investigating a unique research question.
Of the 15,000 patients who donated their genomic and clinical data to Phase 1 of the resource, at least 1,500 had results of their genomic analysis returned to their care teams to help inform their treatment. This is precision oncology in action, made possible through Network resources and expertise.
Several Network-funded projects are also investigating various aspects of precision oncology implementation and delivery, generating the knowledge and evidence needed to apply precision cancer care at scale and equitably.
Canada is a leader in cancer research and policy; however, jurisdictional and geographic barriers mean that research efforts are often siloed in individual institutions or distinct regions, and are typically concentrated in larger urban centres.
To overcome this gap, the Network has created a unified approach to help ensure that resource, knowledge and data can be accessed by centres across the country, helping to make precision oncology research and care feasible in centres where, just a few short years ago, it would have been out of reach. In addition to this, strategic investments to strengthen capacity at smaller centres serving diverse, rural and remote communities have also been made—expanding access to research participation and state-of-the-art cancer care. This includes direct investments in places such as Prince George, BC; Kingston, ON; Windsor, ON; Moncton, NB; and St. John's, NL.
Forty-five years ago, Terry Fox said he wanted all Canadians to be a part of his Marathon of Hope. He really meant all Canadians, including Indigenous Peoples, Canadians living in rural and remote regions, new Canadians and other minority and racialized groups, who collectively experience poorer cancer-related outcomes. The Marathon of Hope Cancer Centres Network is ensuring that the research it supports is representative of the full spectrum of Canadian populations — enabling research and results that are inclusive, representative and fair so that everyone can benefit.
The Canadian Spectrum Working Group, chaired by Drs. Nadine Caron (First Nations Health Authority Chair in Cancer and Wellness at UBC and director of the Northern BC Biobank Initiative), Robin Urquhart (Dalhousie University) and Jean-Marc Bourque (Centre hospitalier de l’Université de Montréal), was formed to develop inclusion strategies for equity-deserving populations within Network activities. The group has developed the MOHCCN Underserved and Underrepresented Populations Guideline to provide standardized definitions for these populations, providing a basis from which to create strategies to respectfully and meaningfully engage with relevant communities.
The Network is continuing to expand across Canada, with a particular emphasis on creating new partnerships with smaller cancer centres and community hospitals serving rural, remote and Indigenous communities as well as with health organizations with similar objectives and values. Consultations and engagement with diverse stakeholders are guiding a better understanding of their needs and priorities and helping to identify new partnership opportunities as well as existing programs successfully promoting health equity.






“The Network is building the foundation for how precision medicine can be done across Canada and how it can, hopefully, be implemented as standard of care. There is a saying that “a high tide floats all boats” and that is what the MOHCCN has done for cancer research in Canada.”
- Dr. Sherri Christian, cancer researcher and professor at Memorial University of Newfoundland
Precision oncology is already bringing hope to some cancer patients across Canada. Below are some stories from patients who are benefitting from this innovative approach to cancer treatment, and who motivate us to continue working to bring life-saving care to more Canadians.

Over the last five years, we have created a pan-Canadian Network that is already impacting the lives of Canadians with cancer. With renewed funding from the Government of Canada, Phase 2 will see us bring precision oncology to more Canadians, improving equitable access to life-saving treatments and gathering the evidence needed to guide value-driven adoption by healthcare systems.





Forty-six years ago, Terry Fox pushed us to dream of a world where the suffering caused by cancer was a thing of the past. There is still much work to do to make his vision a reality. But if Phase 1 has shown us anything, it is that when we come together with a shared purpose, there is no limit to what we can achieve.
In 1980, Terry Fox started a marathon against cancer. Together, we can FINISH IT.